Time out procedure upmc8/9/2023   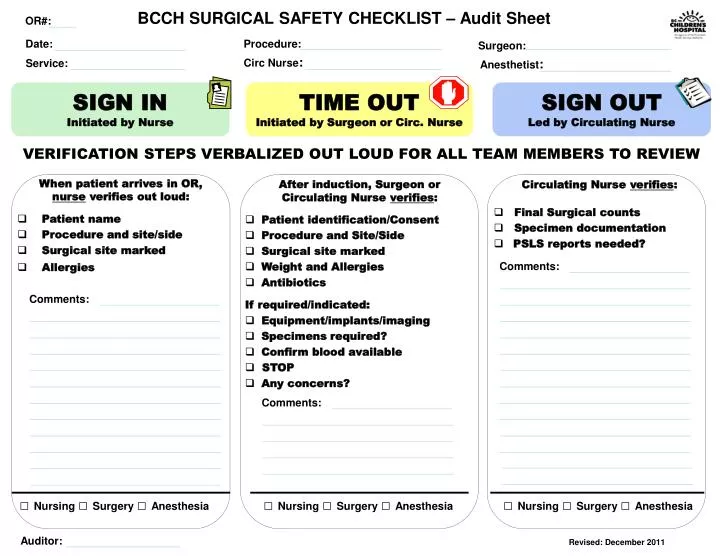
“We had created many, many, many different siloed roles around discharging patients from the hospital,” she says. Add in the necessary steps to transfer a patient to a rehab or skilled nursing facility or send a patient home, perhaps with remote patient monitoring services or scheduled follow-up appointments, and patients weren’t seeing daylight until late afternoon. Minnier says the patient discharge process had grown cumbersome over time, adding in a variety of check-offs and approvals that built up like gravel gathering along the edges of a streambed. “There’s a lot that we’ve been able to improve, and I really think we’re only scratching the surface of what we can gain.” “Our people have become a blended team … with a new boss,” says Tami Minnier, MSN, RN, FACHE, FAAN, the Pennsylvania health system’s senior vice president of health services and chief quality & operational excellence officer, and the driving force behind the new strategy. The process has shaved 3–4 hours off patient discharge times, improved consult and referral protocols, and boosted HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems) scores by almost 10%. Recognizing the logjams that can occur when leaving the hospital, UPMC has launched a new patient discharge process that consolidates decision-making under one clinical care coordinator and creates a platform for data gathering. That, in turn, might make it less than appealing for patients, thus affecting both satisfaction and engagement metrics. Patient discharge can be a particularly nasty pain point for hospitals, involving several people from several departments and data from a variety of sources. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
